SALUS - an evidenced-based approach
Our research showed that HIV communication at clinics is mostly ineffective. Health care workers use didactic methods that tell young people what to do, that often results in misunderstanding and confusion.
Our research showed that HIV communication at clinics is mostly ineffective. Health care workers use didactic methods that tell young people what to do, that often results in misunderstanding and confusion.

Belonging is at the heart of young people's motivation
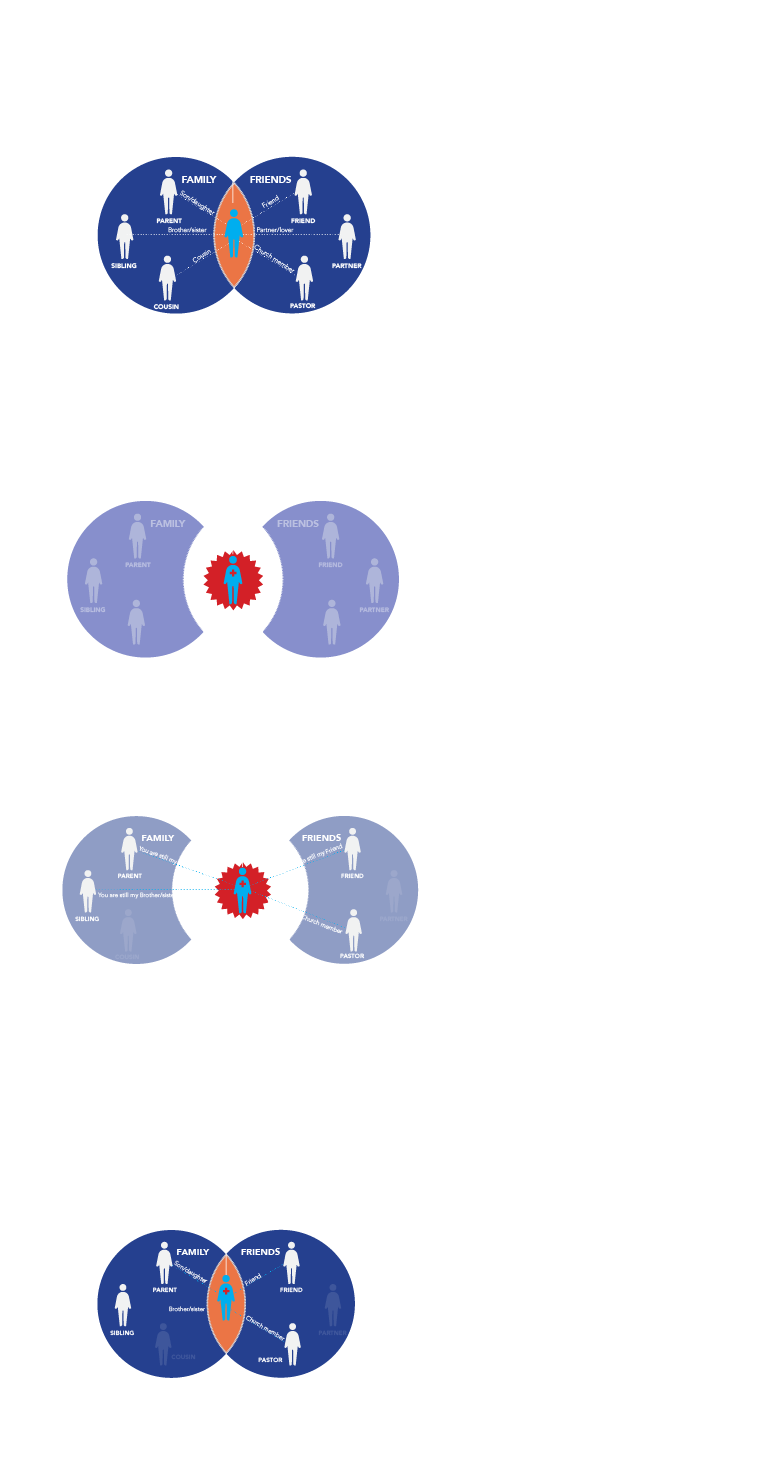
Because young people felt so traumatised by their diagnosis they said that they could not hear the messages that clinicians spoke to them. At this juncture treatment information was not their priority.
To help support them at this difficult moment,participants said that they wanted to listen to other young people’s stories of how they had re-connected and had moved beyond the trauma of diagnosis to living normal full lives.
Because young people felt so traumatised by their diagnosis they said that they could not hear the messages that clinicians spoke to them. At this juncture treatment information was not their priority.
To help support them at this difficult moment,participants said that they wanted to listen to other young people’s stories of how they had re-connected and had moved beyond the trauma of diagnosis to living normal full lives.
A case study film was made that was usedduring pilot funded by ViiV.
A case study film was made that was usedduring pilot funded by ViiV.
Young people said that an animation would help them tobetter understand adherence. In response, an animation was produced explaining the concepts of viral load andCD4 count. Other details of the visual representation were developed in consultation with clinicians and young people.
Young people said that an animation would help them tobetter understand adherence. In response, an animation was produced explaining the concepts of viral load andCD4 count. Other details of the visual representation were developed in consultation with clinicians and young people.

The pilot animation was piloted to groups of young people at one of the clinics by a young man who himself was living with HIV.
During presentations of the pilot animation young peopletalked passionately about their own experiences, including the loss of family members, friends and communitymembers to HIV in the past. Many of them had not done so before and found it very helpful. They also asked
many questions about HIV and treatment, and a dialogue developed. This kind of exchange was valued greatly
by them. Findings showed that communication will be more effective in settings that provide a space for sharing and learning of this kind than in conventional one-way transmission of information.
The pilot animation was piloted to groups of young people at one of the clinics by a young man who himself was living with HIV.
During presentations of the pilot animation young peopletalked passionately about their own experiences, including the loss of family members, friends and communitymembers to HIV in the past. Many of them had not done so before and found it very helpful. They also asked
many questions about HIV and treatment, and a dialogue developed. This kind of exchange was valued greatly
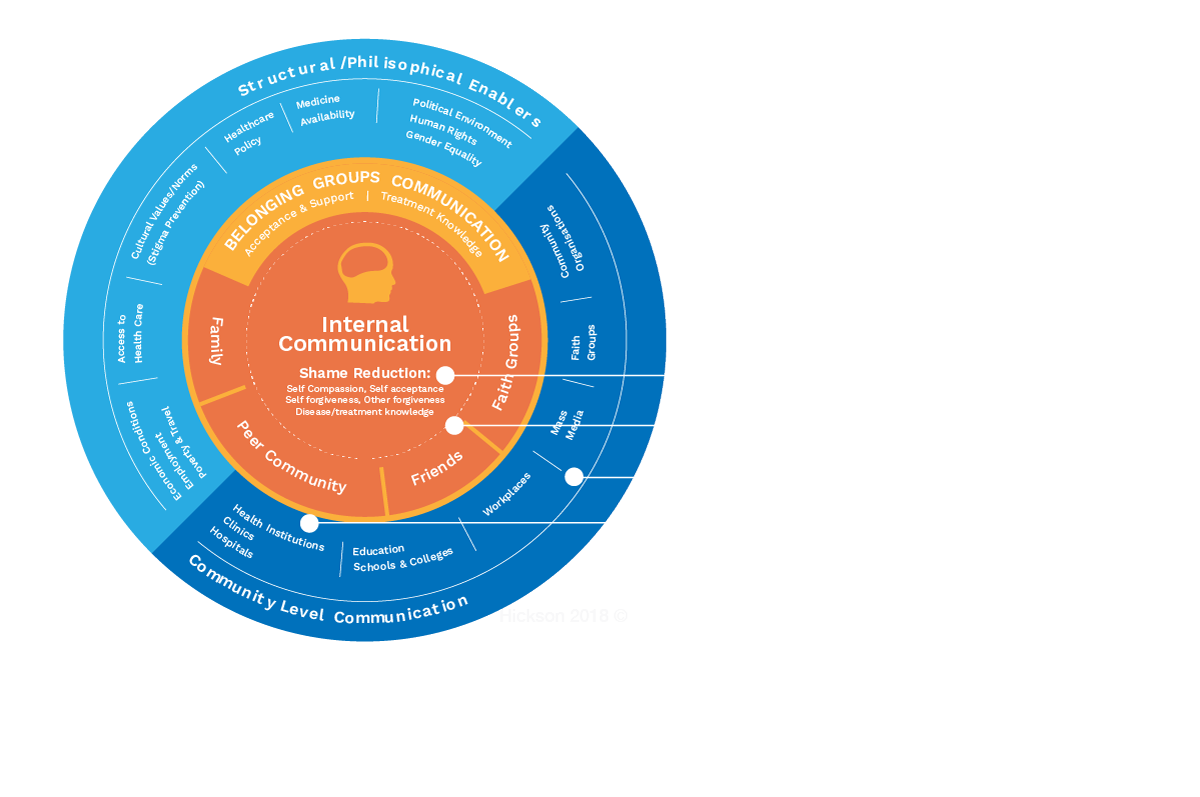
The ecology of HIV psychosocial behavioural communication